AUBURN MCINTYRE
Auburn McIntyre is the Haemophilia Physiotherapist at the Women’s & Children’s Hospital, Adelaide
In this article we will be looking at particular musculoskeletal matters that can occur in all children and adolescents, not just those with haemophilia. These conditions cannot occur once you become an adult as they relate to growth and growing bones and muscles.
Children’s bones are softer and more pliable than adult bones. As a result, the bones of younger people can bend and children have “green stick fractures”, something adults can no longer have. A little like a young tree, the bark can peel down, rather than cleanly snap.
Secondly, the long bones (e.g., the thigh, shin and arm bones), have growth plates at both ends. The long bones become longer and wider with growth. The bones of the lower leg grow most, noticeably around the knee.
Some bones, like the pelvis, knee and heel bones, have special growth plate areas where strong muscles and ligaments attach, called an “apophysis”. The growth plates are weaker than the ligaments. Occasionally a strong force can pull strongly at the anchor point causing pain, swelling and weakness. This saves the ligament and muscle from being damaged but is painful and causes weakness of the muscle. Apophysitis sites are discussed a little later.
Strong skeletal muscles are essential for good movement. Poor muscle development and poor fitness is associated with poorer long term health. It is not possible to bulk muscles until puberty, hence it is recommended free weights and a variety of activities rather than machines and specialized sports are employed prior to puberty (approx. 10-14 years). A great variety of activities establishes the framework for good strong muscle fibre development.
Education and awareness of growth spurts is important as fitness is needed for long term health. Gaining skills through a variety of sports before a child is 10 years old helps skills and works all muscles. It is important to be aware of growth spurts but not worry about them.
Tell your physiotherapist and doctor if your child is growing rapidly.
Work-life pressures can mean it is difficult for parents to provide their child with a large variety of activities but variety enhances strong development of many leg, arm and trunk muscles and assists the body to develop co-ordination, balance and strength.
Adults shrink, only children grow.
A growth spurt, around 10-15 years in boys, poses some risks to children and adolescents as bones grow at different rates to muscles. The early part of a pre-pubertal growth spurt is marked by rapid growth of the legs. The difference between the bone and muscle growth can create problems with general flexibility, co-ordination, muscle power and strength.
Children and adolescents can become clumsy during periods of growth. They are more at risk of injury.
Mechanical stress (tractioning, pulling and tugging), often due to over-use by training the same muscles too frequently, can cause over-use pain. This is called traction apophysitis and can occur at sites commonly affected by haemophilia, such as the elbow, ankle and knee. A sudden, strong and forceful action of a muscle that attaches to the soft area of the growth plate may cause that attachment area to pull off completely. This is known as an avulsion fracture.
In the pelvic area this can be when muscles of the trunk attach at the iliac crest. If they are over worked or worked suddenly, pain can occur along this area. The Ischial tuberosity has the hamstring muscles attached to it. Over stretching or a sudden movement against force can cause an avulsion fracture.
The anterior superior iliac spine has the sartorius muscle, a hip-lifting (flexor) and turning muscle which can also detach part of the bone when the leg kicks a heavy wet ball or the hard ground.
Physiotherapists often want to know “how the injury happened” and “what where you doing when…..”. This is to try and determine if the sudden pain is a bleed or something else. Sometimes X-rays are required to determine if the pain is due to a fracture. Many things can cause pain, not just a bleed.
At the knee there are two common sites that can become sore and painful. The names attached to these injuries are Osgood-Schlatter disease and Sinding-Larsen disease. They are locally painful, can be sore with running, when touched and working the quads (quadriceps femoris) muscles. These injuries are usually due to over-use and tight muscles.
Down at the foot, the heel reacts to tight calf muscles pulling on bone, for example, with running, jumping or even walking. This can result in pain, swelling and is often worse after rest, again usually when muscles are tight pulling and tugging occurs. Local pain, sometimes stiffness and swelling can result.
The above injuries relate to tight muscles pulling on softer bony growth plates, during a period of growth, or a sudden action of the muscle which can pull the soft bone off its harder base. They generally cause local tenderness, swelling or pain, not whole knee swelling as in a bleed – for example, a local area of pain at the heel or under the arch, not the whole ankle. They can hurt and lead to you being unable to lift a leg or walk. They require proper assessment.
Factor replacement therapy may make some difference; due to perhaps some bleeding of the body part involved but it will not be the same as in a bleed to a joint or muscle. The problem will reoccur and not settle with re-use.
Children with suspected bleeds should always be reviewed. Growth spurts are times when other issues arise and proper assessment is critical.
True joint bleeds improve with factor replacement therapy. They require proper PRICE (Protection Rest Ice Compression Elevation) and rehabilitation afterwards to improve the muscle power, strength and flexibility that is always lost after a bleed.
A period of relative rest and specific exercises are required for apophysitis and growth plate injuries. They may even require an orthopaedic review and an X-ray.
Other than psoas muscle bleeds, the hip region is commonly less problematic for people with haemophilia. A bleed into the ankle, knee or elbow is much more problematic.
However, in children the hip region can be a site of other musculoskeletal issues.
Infections can occur in this area and also in other joints. This may be after a viral illness such as a cold or ear infection or even a recent open wound. A child might limp or complain of groin or knee pain and have restricted movements. Commonly the 3-10 year old age group is affected. Adults can also get joint infections but many types are more common in children.
Children should never have a temperature or be unwell with a haemophilic bleed.
Boys, 10-15 years old, are 60% more likely than a girl to develop a slip of part of the hip bone, (a slipped upper capital femoral epiphysis). This can occur suddenly and they will have a quick onset of pain and loss of movement and function, or it can occur gradually over time. Both result in restricted hip movements. Sometimes the leg may appear shorter and the child will limp. There is a heightened risk if children are overweight. Treatment is generally surgical.
Some children will complain of knee pain when the problem is actually in the hip joint. Both joints should always be checked.
Boys, 4-10 years old, more than girls can develop Perthes, another hip condition with limping, persistent pain and restricted hip movements. Perthes often occurs gradually.
If a child has a slipped upper capital femoral epiphysis or Perthes, they will not respond to factor replacement therapy. If they have a bleed, children should always improve and continue to improve if given factor.
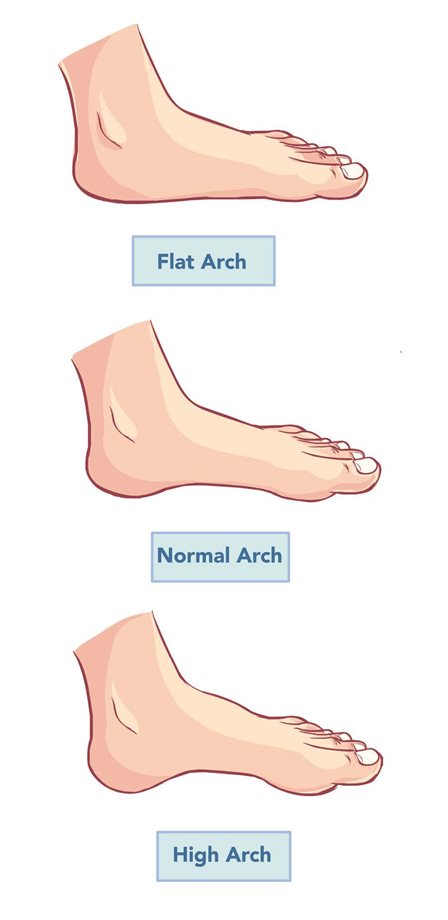
Flat feet, which are normal in children until around 5-7 years, can sometimes lead to stiff feet in adolescence. Why this occurs in unknown and it is not common. When asked to stand on tip toes, children with stiff feet don’t show the natural arch that most people get. An orthopaedic review may be required if their feet are causing problems, have calluses etc.
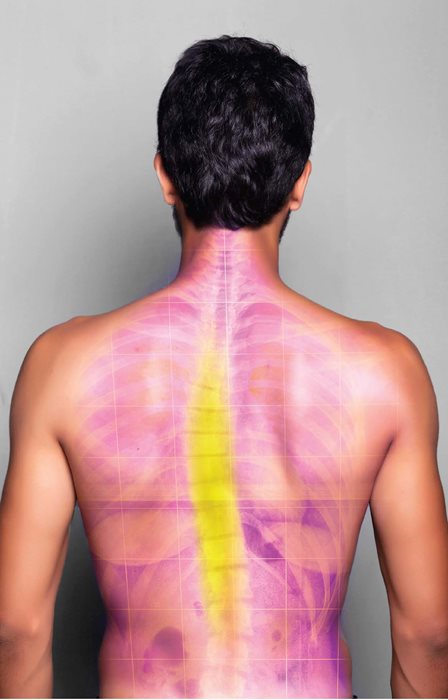
Scoliosis
Children’s spines are growing so posture is constantly changing. More girls than boys develop a sideways curve in their spine called a scoliosis but boys can become very round shouldered or kyphotic. They can also develop a scoliosis. These spine conditions may become problematic if they continue to develop with growth. Often they are hidden under clothes so have a look at your child’s spine in summer when they are less likely to have so many thick layers on.
Enjoy watching your child grow. It’s an amazing process, full of joys as they become better at skills and conquer new activities.
Be aware that all aches and pains may not be bleeds. Take note of the acqua bold alert text …….
Contact your HTC if the “pattern” of the problem is different to a normal bleed or if the problem doesn’t settle or if the problem reoccurs. Act, don’t wait!
Haemophilia Foundation Australia acknowledges the Traditional Owners and Custodians of Country throughout Australia, the land, waters and community where we walk, live, meet and work. We pay our respects to Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples.
Sign up for the latest news, events and our free National Haemophilia magazine