GRAINNE DUNNE
Grainne Dunne is Clinical Nurse Consultant, Haemophilia, at Sydney Children’s Hospital
Our mouth is a most wonderful and interesting part of our body. It’s the first step in breaking down food to allow us to then to swallow our food; we taste everything using our mouth; it’s important in the process of breathing; we communicate with our mouths to talk, smile, show emotions; and it’s an important way to show our loved ones how we care about them with that simple but important kiss.

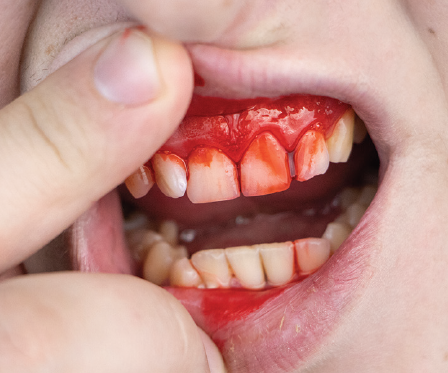
However, it’s also highly vascular…. which means it has many, many blood vessels that are needed to perform all the above amazing functions. When you have a bleeding disorder of any type (haemophilia, von Willebrand disease, inherited platelet function disorder or another rare bleeding disorder), injury to these blood vessels can lead to a lot of blood loss and at times can be challenging to stop.
1. As this is a highly vascular area, there are a lot of blood vessels to leak out blood when injured.
2. Saliva in the mouth, required to break down food and to keep our mucus membranes becoming too dry, contains enzymes and uric acid. These elements are not good friends with a newly developing clot, particularly in a bleeding disorder when the clot is difficult to make to begin with. Saliva can play a part in breaking down a weak clot which leads to the initial injury site re-bleeding again.
3. Chewing and movement of food around the mouth, particularly hard or bulky foods, can knock at and disturb a developing clot and thus restart the initial bleed again.
4. Humans are curious by nature. When we feel something unusual in our mouth, we naturally want to investigate it. In fact, for many of us, it’s difficult to consciously leave it alone. So, whether consciously or subconsciously, we often push our tongue over the injury site to ‘examine/investigate’ that unusual feeling in our mouth. In some cases, it may be an over-curious finger that finds its way into our mouth investigating that tender injury site – especially in children. Such ‘examination’ or ‘investigation’ can disturb a tender and developing clot and of course… restart the bleed.
5. Objects in the mouth: In young toddlers and babies, toys and other objects are notorious for finding their way into the mouth. A child at this age often uses their mouth to investigate an object – which is not what one wants when a clot is trying to form and harden after a bleed has recently occurred. The older and more mature child (and adult!) can accidently hit the injury site using their eating utensil e.g., fork, spoon, and again disturb the delicate clot development.
Ice! It’s simple but its effective.
Do I need to tell my haematologist that I am having mouth surgery?
YES!
Prevention is always better than cure!Dental plaque is a sticky, acidic film of bacteria and food debris on teeth, which everyone gets – it’s a normal process. However, a build-up of plaque is bad for your teeth and if not removed will form tartar. Plaque and tartar increase your risk for dental cavities, tooth decay, gum disease, reseeding gums, and other harmful dental problems, leading to tooth loss and then the need for dental surgery.

To help between dental visits, you can remove some tartar at home. Here are a few tips.
Australian Haemophilia Centre Directors’ Organisation. A consensus statement on the dental treatment of patients with inherited bleeding disorders, July 2010. Accessed 7 August 2023.HealthDirect – Dental care
Haemophilia Foundation Australia acknowledges the Traditional Owners and Custodians of Country throughout Australia, the land, waters and community where we walk, live, meet and work. We pay our respects to Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples.
Sign up for the latest news, events and our free National Haemophilia magazine