SUZANNE O'CALLAGHAN
Suzanne O'Callaghan is HFA Policy Research and Education Manager
With new haemophilia treatments for adults and children available now across Australia, the 2021 Conference was a great opportunity to discuss how the new treatments impact on bleeding episodes and how to manage bleeds when they occur.
This is a summary of the discussion, but if you are interested you can still watch the full session. Visit www.haemophilia.org.au/conference21 for more information.
Concurrent 1 – Managing bleeds under current new treatments
20th Australian Conference on Haemophilia, VWD and Rare Bleeding Disorders
Chair ~ Jane Portnoy
The impact of new haemophilia treatments on people with haemophilia, parents and health professionals ~ Jane Portnoy
Short personal stories
Understanding bleeds under new treatments ~ Dr Julie Curtin
Physiotherapist perspective ~ Alison Morris
Nursing perspective ~ Joanna McCosker and Beryl Zeissink
The benefits of the new treatments have been welcome, but there is no doubt that the changes involved can be substantial.
What have these changes meant to individuals? Jane Portnoy, Haemophilia Social Worker at the Ronald Sawers Haemophilia Centre in Melbourne, opened the session with a snapshot of experiences among adults and children with haemophilia cared for by Haemophilia Treatment Centres (HTCs) in Australia. She pointed out that experiences can vary: for many on prophylaxis it was a huge relief not to have to infuse into a vein and infuse so often; others were more cautious and wanted to wait to get ready to start the new treatment; and some have experienced disappointment if the new treatment did not work out for them. There were challenges with learning the new processes for administering the treatment, but more opportunities – to travel, to be with friends and family, to take on new sports and activities.
A powerful part of the session was hearing from people with haemophilia and parents about their experiences with the new treatments.
For Lenny non-factor therapy was an exciting and very welcome change: infusing only once a week, collecting his treatment product from the pharmacy, the independence of being able to administer his own treatment instead of relying on his family, and so many new aspects to his life – finishing his university degree and looking for employment, singing with a community choir and volunteer community work.
Leah gave a parent’s perspective. Her small daughter has severe haemophilia and had experienced both an extended half-life therapy and a non-factor therapy. Although she is very active, her daughter has started primary school with very few bleeds and hospital admissions. Leah commented that it is harder now to know how to recognise a bleed, so they err on the side of caution. ‘We feel really fortunate to live in this era and in this part of the world – because we know not everywhere has access to these treatments. She can live, she can go to school, every party doesn’t end up in a hospital admission, like it used to.’
Bruce is in his 70s and gave an account of his treatment experience with extended half-life factor for prophylaxis as an older man. Prophylaxis had made a great difference to controlling his bleeds, but for Bruce one of the greatest positives of moving from standard prophylaxis to a longer acting factor was the condition of his veins – treating only once every 6 days instead of 3 times per week. He also felt freer travelling, with a much smaller volume of treatment product to carry with him.
Understanding and managing bleeds with extended half-life and non-factor therapies such as Hemlibra® is also new territory. Dr Julie Curtin is HTC Director at the Kidz Factor Zone at Westmead Children’s Hospital, Sydney, and provided an expert and very accessible walk through the science and the issues.

Extended half-life factors (EHLs): Dr Curtin explained that although EHLs can reduce the number of infusions, every person reacts a little differently and this needs to be measured in the individual through pharmacokinetic (PK) studies. Other important factors in an individual’s treatment plan:
If patients using EHLs have a breakthrough bleed, the bleed treatment may include the EHL. Treating serious bleeds can involve a more complex treatment plan and close monitoring of factor levels is critical.
Non-factor products – Emicizumab (Hemlibra®): outlining the action of emicizumab, Dr Curtin explained that it worked like factor VIII, bringing together factor IX and factor X to continue the clotting pathway.
Although the new treatments have reduced the risk of injury and the number of bleeds, injuries and bleeds still occur. In the Q&A that followed, physiotherapist Ali Morris and haemophilia nurses Joanna McCosker and Beryl Zeissink outlined some of the issues for people with haemophilia on new treatments and were joined by Dr Julie Curtin in a panel discussion.
Ali Morris is the Senior Musculoskeletal Physiotherapist at Perth Children’s Hospital and her experience brought a real sense of how the issues play out for young people. She pointed out:
Ali walked through some key aspects of rehabilitation – the process of healing and decisions involved in returning to sport and activity safely.
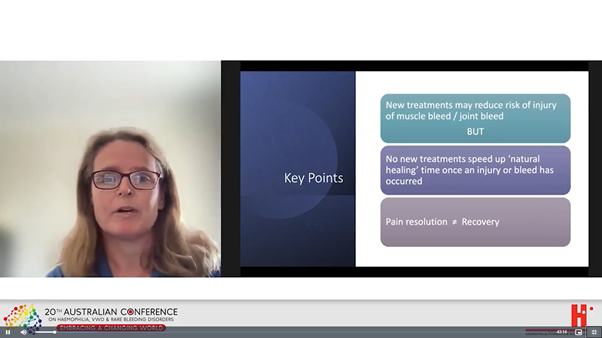
When to contact the HTC is a common question now with the new treatments. Jo and Beryl are haemophilia nurses at the paediatric and adult Haemophilia Treatment Centres in Queensland and drew on their common experience and suggestions from their colleagues to answer this question. They explored in particular:

Questions from viewers prompted lively panel discussion about treatment choice, identifying bleeds, bleed treatments, playing sport and preparing for school camp or holidays. They also looked at some of the psychological challenges of changing to a subcutaneous treatment, personal choice and the process of getting ready for change.
The Q&A finished with some questions about gene therapy and bleed treatments and the impact of the new treatments on physical activity and independence – and overall confidence in living life with haemophilia.
Haemophilia Foundation Australia acknowledges the Traditional Owners and Custodians of Country throughout Australia, the land, waters and community where we walk, live, meet and work. We pay our respects to Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples.
Sign up for the latest news, events and our free National Haemophilia magazine